Increasing Community and Facility HIV Testing in Mozambique
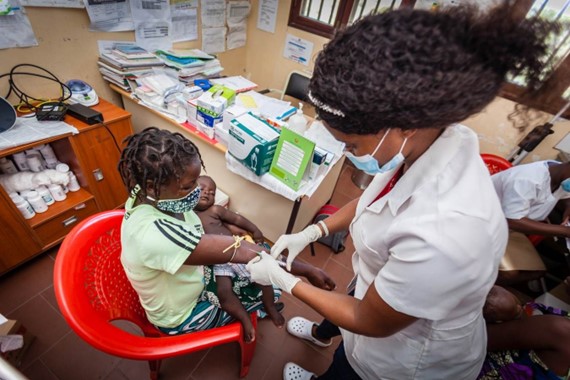

For Armando, a 35-year-old onion seller in the province of Niassa in northern Mozambique, the news could have been tragic. Male Champions, the Efficiencies for Clinical HIV Outcomes (ECHO) project’s male volunteers who perform outreach to other men for HIV testing, had visited the market where Armando works. They encouraged him to take a free HIV test at a health clinic, and despite the stigma attached to HIV in Mozambique, Armando (a pseudonym) and his wife, Paula, took the test. The results weren’t what they had hoped.
But the positive test results weren’t the end of the story. Community activists visited Armando and his wife at their home and counseled the couple on the importance of adhering to their treatment regimen. The ongoing supportive relationship that developed persuaded Armando and his wife to take their medication—and that probably saved their lives. “They are also my friends, and they always visit me,” Armando says of the Male Champions. “When I’m not at home, they come to the market.”
The Male Champions and community activists are an important part of ECHO, which slowly but surely is tackling the HIV and AIDS epidemic in Mozambique. HIV is the second leading cause of death in the country, which has an estimated HIV prevalence among adults of 12.6 percent, the eighth highest rate in the world.
The USAID-funded and Abt Global-led ECHO project aims to help Mozambique achieve the UNAIDS 95-95-95 global target: 95% of all people living with HIV know their HIV status, 95% of all people living with HIV receive sustained antiretroviral therapy (ART), and 95% of patients on ART are virally suppressed or have undetectable amounts of the HIV virus.
Key elements of the ECHO initiative include investing in scaling up HIV testing and increasing the number of patients starting ART. The investments target health facilities and community outreach. Referrals are a critical link between testing and treatment. When health facility staff provide self-testing kit instructions to at-risk community members, they share their contact information. When people test positive, they can use this contact information to learn how to get treatment.
Since ECHO’s inception in 2019, the project has sought to reduce the number of patients who test positive but don’t get treatment, which was as high as 33%. Why don’t people get treatment? Many patients do not have time to go through the process to access it or are worried about potential side effects. Additionally, fears of stigma and discrimination can create a psychological barrier to accepting one’s diagnosis and reaching treatment. Some spiritual beliefs about witchcraft also prevent linkage to treatment.
When patients don’t promptly connect with treatment, community activists contact the patients to let them know how to get access to ART and refer them to counselors who help them accept their diagnosis. This outreach to patients creates a clear next step for people who have tested positive. Now nearly 100% of patients testing positive initiate ART.
Mistrust of the healthcare system and stigma may discourage some people from getting tested in the first place. For that issue, ECHO employs a different tactic: dispatching community health workers to encourage HIV testing in non-healthcare settings such as schools, universities, churches, markets, football fields, interdistrict bus stops, fairs, election events, and other gathering places. ECHO distributes self-testing kits to key populations, including sex workers and at-risk members of the LGBTQ community. ECHO also doubled the number of self-testing kits distributed at the community level and began stockpiling tests to avoid shortages.
Health facilities also missed opportunities for testing. In response, ECHO rolled out testing guidance to providers that emphasized casting a wide testing net—testing all patients rather than targeting smaller groups. This aligned with a shift in the U.S. President’s Emergency Plan for AIDS Relief’s strategy. Additionally, health facilities dedicated counselors to at-risk children to ensure consistent re-testing for them, as transmission can occur at any stage of development. Health units also ensured patient privacy by creating small, enclosed spaces in clinics, known as testing corners. To address stockouts and supply chain issues related to testing kits, ECHO monitors the inventory of its facilities to ensure adequate supplies.
As a result of ECHO’s efforts, the number of people who tested for HIV in ECHO-supported facilities grew from Quarter 1 to Quarter 3 of 2023. The number of people who tested positive in the four provinces ECHO supported increased by five percent from 14,746 in Quarter 1 to 15,442 in Quarter 3. Like Armando and his wife, they learned of their situation—and could get life-saving treatment.
Read More
Infectious Diseases & Global Health Security in Sub-Saharan Africa

Bolstering Global Health Security in a Changing Environment
Environmental hazards require adaptive global health security strategies.

Beyond COVID-19: What Global Health Security Will Look Like
As leaders focus on pandemics and global health security, they should look at three related items: other diseases, social determinants of health, and logistics.

Improving Immunization Programming in Mozambique
An analysis of Mozambique’s 2015 immunization spending reveals that despite adequate resources and increases in immunization coverage, challenges to the immunization program persist. In addition to examining the efficiency of the immunization program, Mozambique would benefit from efforts to report and compile immunization spending data more effectively.This policy brief and the underlying health accounts exercise have been supported by Abt Global, through a grant secured from the Bill and Melinda Gates Foundation.Also available in Portuguese.

A Concise, Health Service Coverage Index for Monitoring Progress Towards Universal Health Coverage
There is a growing international commitment to universal health coverage (UHC), but limited means to determine progress towards that goal. The authors developed a practical index for capturing health service coverage – a critical dimension of UHC -- that was more inclusive than previous methods.The approach moved beyond common indicators of service coverage focused on infectious diseases and maternal and child health, to include information on necessary health inputs. The resulting, balanced, composite index of health service coverage demonstrated promise as a metric, likely to discriminate coverage levels between countries and regions. An important number of service provision indicators were correlated, therefore a reduced set of services performed well as a proxy for the full set of available indicators. This parsimonious index is a start toward simplifying the task of policy-makers monitoring progress on a key domain of universal health coverage.
